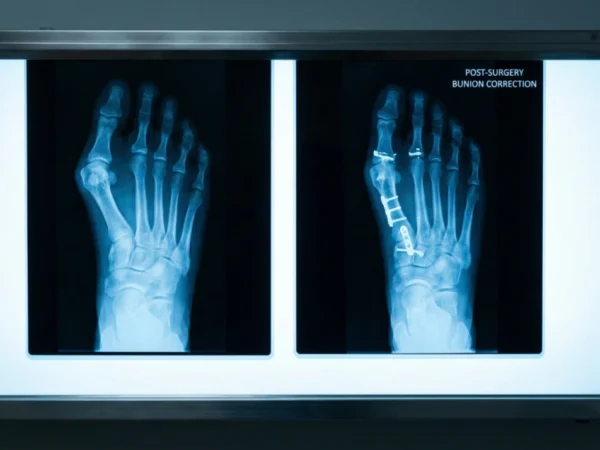
The most effective clinical treatment for bunions, known medically as hallux valgus, involves a dual strategy: the use of custom Foot Orthotics to redistribute mechanical stress and Foot and Ankle Surgery to physically realign the skeletal structure. While conservative measures such as padding and orthotics can effectively manage symptoms and slow progression, surgical intervention is currently the only radical method to correct the bone deformity and restore normal joint alignment.
Anatomical Pathophysiology and the Primary Bunions Cause
In the American medical community, a bunion is defined as a complex, three-dimensional progressive deformity of the first ray of the foot. It is characterized by the medial deviation of the first metatarsal bone and the lateral deviation of the big toe (hallux) toward the other digits.
Identifying the Reasons for Bunions
The reasons for bunions are multi-faceted, involving a breakdown in the balance of muscles and ligaments that stabilize the first metatarsophalangeal joint (MTPJ).
-
Genetic Predisposition: Up to 70% of patients have a documented family history of the condition.
-
Biomechanical Instability: Conditions like flat feet (pes planus) lead to hyperpronation, placing excessive stress on the medial aspect of the foot.
-
Footwear Choices: Chronic use of high heels or narrow-toed shoes serves as a significant bunions cause, forcing the toes into an unnatural “bowstring” position that stretches supporting ligaments over time.
Early Recognition and Diagnostic Standards
Early intervention is critical to avoiding invasive procedures later in life. An early sign of bunion formation typically includes intermittent discomfort in narrow footwear or a slight redness and swelling at the base of the big toe, often indicating the onset of bursitis.
Clinical Classification and Severity
The clinical severity of a bunion is categorized based on these specific measurements:
-
Mild Deformity
-
HVA is less than 20°.
-
IMA is less than 11°.
-
Symptoms are often limited to periodic discomfort when wearing narrow shoes.
-
-
Moderate Deformity
-
HVA is between 20° and 40°.
-
IMA is between 11° and 16°.
-
This stage is characterized by constant pain, inflammation, and limited joint mobility.
-
-
Severe Deformity
-
HVA is greater than 40°.
-
IMA is greater than 16°.
-
This stage often involves the overlapping of toes, significant gait disruption, and secondary issues like hammertoes.
-
Conservative Management and Supportive Footwear
Selecting Shoes Comfortable for Bunions
Finding shoes comfortable for bunions is the first line of defense recommended by the American Academy of Orthopaedic Surgeons (AAOS). Ideal footwear should feature:
-
A Wide Toe Box: To prevent compression of the deformity.
-
Soft Upper Materials: Flexible mesh or soft leather that accommodates the protrusion.
-
Low Heels: Heels higher than $2$ inches ($5$ cm) shift weight to the forefoot, aggravating the joint.
For those managing shoes, bunions can be further stabilized by using supportive shoes for foot pain paired with custom-molded Foot Orthotics. These devices help control pronation and reduce the mechanical load on the first MTPJ.
Modern Surgery on Bunions and Clinical Innovations
When pain limits daily activity and conservative measures fail, surgery on bunions is considered the most effective solution. In the US, more than $450,000$ corrections are performed annually.
Surgical Standards in 2026
-
Lapiplasty® 3D Bunion Correction: A breakthrough technology that addresses the rotation of the bone rather than just the angle. This reduces the recurrence rate to approximately $3\%$, compared to $30\%$ with traditional methods.
-
Minimally Invasive Surgery (MIS): Surgeons perform the correction through tiny $3$ mm punctures. This results in minimal scarring, reduced post-operative pain, and a faster return to daily life.
Bunion Surgery Recovery
The bunion surgery recovery timeline has been significantly optimized. While traditional procedures often required weeks of total rest, modern 3D techniques allow many patients to begin protected weight-bearing in a specialized boot within $3$ to $10$ days. Full recovery and a return to regular footwear typically occur between 3 and 6 months.
The Digital Frontier: AI and Economics in US Podiatry
Cost and Insurance Coverage
In the US, the cost for surgical treatment for bunions ranges from $3,500 to $12,000 per foot.
-
Medicare Part B: Typically covers 80% of the cost for medically necessary procedures.
-
Medicare Advantage: Patients should be aware of “Prior Authorization” requirements, which saw a 13% denial rate in 2024, often requiring professional audit and appeal.
| Treatment Level | Primary Goal | Recommended Intervention |
|---|---|---|
| Early/Mild | Prevent progression | Foot Orthotics & wide toe-box shoes |
| Moderate | Pain management | Physical therapy & anti-inflammatories |
| Severe | Full correction | Foot and Ankle Surgery (3D or MIS) |
Frequently Asked Questions
What exactly is a bunion and what is the underlying cause?
Can I get rid of bunions without surgery?
Why are bunions more common in females?
Women are affected three times more often than men due to a combination of factors. These include a genetic tendency toward higher joint laxity, hormonal influences on ligament strength, and the cultural use of restrictive footwear like high heels, which increases pressure on the forefoot.
What are the best shoes to wear for bunions?
Specialists recommend shoes with a wide, deep toe box that does not compress the joint. Look for soft, stretchable upper materials like mesh or premium leather and ensure the heel height is below 2 inches (5 cm) to avoid shifting excessive weight onto the bunion area.
Do toe separators or bunion correctors actually work?
Toe separators and splints can provide temporary symptomatic relief by reducing friction between toes and stretching the joint capsule. However, medical research indicates they do not provide long-term correction of the bone angle. They are best used as a comfort measure rather than a corrective tool.
How long is the recovery time after bunion surgery?
Recovery depends on the surgical technique used. With modern 3D corrections like Lapiplasty, patients may begin protected weight-bearing in a special boot within 3 to 10 days. In contrast, traditional osteotomies may require 2 to 6 weeks of restricted activity. Full recovery and the return to regular shoes typically take between 3 and 6 months.
Does medical insurance or Medicare cover bunion surgery?
Yes, most insurance plans, including Medicare Part B, cover bunion surgery if it is deemed “medically necessary”—meaning the deformity causes chronic pain that limits daily activities and has not responded to conservative care. Patients often responsible for a 20% co-payment, which may be covered by supplemental plans.
References
- Bunions – Symptoms & Causes, Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/bunions/symptoms-causes/syc-20354799
- Bunions – OrthoInfo, American Academy of Orthopaedic Surgeons (AAOS), https://orthoinfo.aaos.org/en/diseases–conditions/bunions/
- Racial Differences in Foot Disorders and Foot Type: The Johnston County Osteoarthritis Project, PMC (National Institutes of Health), https://pmc.ncbi.nlm.nih.gov/articles/PMC3463748/
- Characteristics Associated with Hallux Valgus in a Population-Based Study of Older Adults: The Framingham Foot Study, PMC, https://pmc.ncbi.nlm.nih.gov/articles/PMC4378567/
- Johnson & Johnson Launches VIRTUGUIDE™ AI-Powered Patient-Matched Lapidus System in U.S., J&J MedTech, https://www.jnj.com/media-center/press-releases/johnson-johnson-launches-virtuguide-ai-powered-patient-matched-lapidus-system-in-u-s-to-reduce-complexity-in-bunion-surgery-for-millions
- Treace Announces Peer-Reviewed Publication of Four-Year Results of the ALIGN3D™ Lapiplasty® Multicenter Study, Treace Medical Concepts, https://investors.treace.com/news-releases/news-release-details/treace-announces-peer-reviewed-publication-four-year-results/
- Medicare Advantage Insurers Made Prior Authorization Determinations, KFF (Kaiser Family Foundation), https://www.kff.org/medicare/medicare-advantage-insurers-made-nearly-53-million-prior-authorization-determinations-in-2024/
- Procedure Price Lookup for Outpatient Services (CPT 28297), Medicare.gov, https://www.medicare.gov/procedure-price-lookup/cost/28297