This content is for informational purposes only and does not constitute medical advice. Please consult with a licensed podiatrist for a personalized evaluation and treatment plan. Individual results may vary.
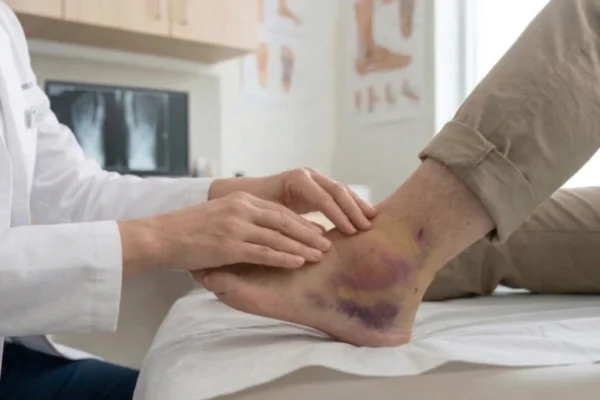
A foot or ankle fracture involves a partial or complete break in the bone, resulting from high-impact trauma, rotational injuries, or repetitive mechanical stress. Primary symptoms include immediate, localized pain, significant ankle injury swelling, visible bruising, and a functional inability to support weight on the affected limb. Immediate clinical evaluation is required if the injury presents with a physical deformity, skin penetration by bone fragments, or neurological symptoms such as numbness or tingling. Early intervention by a specialist is essential to prevent malunion, chronic joint instability, or the rapid onset of post-traumatic osteoarthritis.
For patients in Southern California seeking expert diagnosis and a personalized recovery roadmap, consulting an experienced podiatrist in LA like Dr. Arkady Kaplansky provides access to state-of-the-art surgical and regenerative therapies.
Identifying the Signs of a Broken Ankle and Foot
Acute Physical Indicators
- Audible Trauma: A distinct “cracking” or “snapping” sound at the moment of impact.
- Point Tenderness: Intense pain isolated to a specific bony area, such as the lateral or medial malleolus (the protrusions on either side of the ankle).
- Rapid Edema and Discoloration: Significant ankle injury swelling that occurs within minutes, often followed by deep purple bruising as blood accumulates around the fracture site.
- Mechanical Instability: A sensation that the joint cannot support the body’s weight, or visible misalignment of the foot relative to the leg.
Stress Fractures vs. Traumatic Breaks
Diagnostic Standards: The Role of Imaging
- X-ray of a Broken Ankle: This is the foundational diagnostic tool used to identify the location, direction, and type of fracture (e.g., transverse, oblique, or comminuted).
- Computed Tomography (CT) Scans: Often utilized for intra-articular fractures (breaks that extend into the joint), a CT scan provides a three-dimensional view of the bone fragments, which is vital for an orthopaedic surgeon planning a complex reconstruction.
- Magnetic Resonance Imaging (MRI): While X-rays show the bone, an MRI reveals associated damage to the syndesmosis ligaments, tendons, and cartilage that often accompanies high-energy ankle breaks.
Advanced Surgical and Regenerative Treatment Options
Foot and Ankle Surgery (ORIF)
Platinum Biologics for Bone Healing
Remy Laser Pain Treatment
Post-Traumatic Rehabilitation and Long-Term Support
Specialized Wound Care
Biomechanical Stabilization with Foot Orthotics
- Stabilize the subtalar and talocrural joints.
- Redistribute pressure away from the former fracture site.
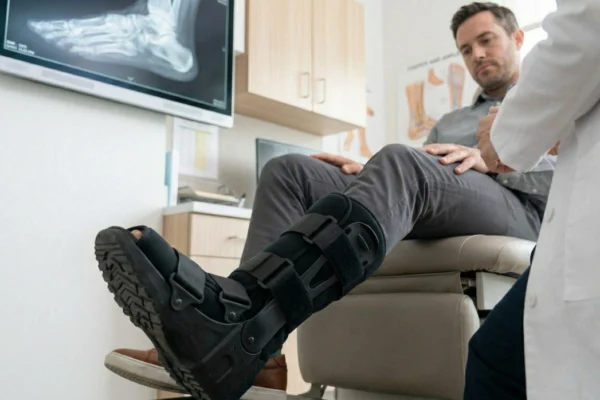
- Correct compensatory gait patterns that may have developed during the weeks spent in a foot fracture boot.
| Treatment Phase | Primary Objective | Key Modalities |
|---|---|---|
| Acute Phase | Stabilization & Pain Control | Casting, Splinting, Remy Laser |
| Surgical Phase | Anatomical Realignment | ORIF Surgery, Platinum Biologics |
| Sub-Acute Phase | Bone Consolidation | NWB (Non-Weight Bearing), Wound Care |
| Remodeling Phase | Functional Restoration | Physical Therapy, Custom Orthotics |
Navigating the Recovery Timeline in Los Angeles
In a metropolis like Los Angeles, where physical activity and mobility are central to daily life, a multidisciplinary approach is vital. Utilizing an orthopaedic surgeon who integrates regenerative medicine with traditional surgical techniques ensures that the bone does not just “close,” but returns to its peak functional state.
Neglecting early broken ankle symptoms can lead to permanent joint degeneration. Seeking professional intervention at the onset of injury is the most effective way to ensure long-term mobility and prevent the chronic pain associated with improperly healed fractures.
Frequently Asked Questions
How can I tell the difference between a severe sprain and a broken ankle?
Is it possible to walk on a fractured foot or ankle?
Does every foot or ankle fracture require surgical intervention?
What is the typical timeline for fractured foot treatment and recovery?
Why are custom foot orthotics recommended after a fracture heals?
References
- American Academy of Orthopaedic Surgeons — https://orthoinfo.aaos.org/en/diseases–conditions/ankle-fractures-broken-ankle/
- American College of Foot and Ankle Surgeons — https://www.foothealthfacts.org/conditions/fractures-of-the-foot
- Mayo Clinic — https://www.mayoclinic.org/diseases-conditions/broken-ankle/symptoms-causes/syc-20370396
- Cleveland Clinic — https://my.clevelandclinic.org/health/diseases/21841-broken-ankle