Finding a permanent bunions cure for a tailor’s bunion (also known as a bunionette) requires a specialized approach. In modern American podiatry, the most effective strategy involves a combination of custom Foot Orthotics to fix biomechanical issues and, when necessary, Foot and Ankle Surgery to physically realign the bone. While home remedies can offer temporary relief, addressing the structural cause is the only way to stop the pain for good and prevent the deformity from returning.
Understanding Tailor’s Bunion: Why That Bump Appears
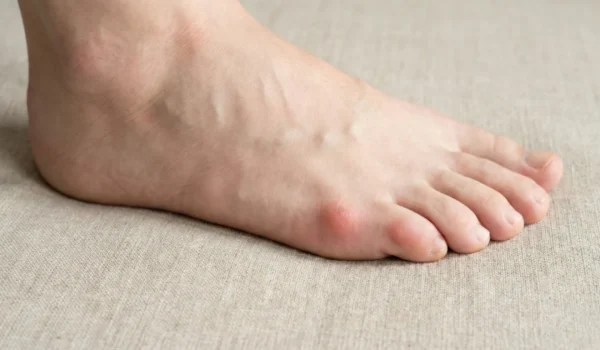
A tailor’s bunion is a structural protrusion of the fifth metatarsal bone on the outer edge of the foot. Historically, it earned its name from tailors who sat cross-legged all day, putting constant pressure on the outside of their feet.
When looking at the primary reasons for bunions, experts point to a mix of genetics and foot structure. If you have flat feet or tend to roll your feet inward (overpronation), your foot “spreads,” forcing the pinky toe bone outward. While tight shoes don’t usually cause the bone to move, they act as a catalyst, irritating the area and causing painful inflammation.
The Role of the Lateral Column
The fifth metatarsal is the “anchor” of the lateral column of your foot. When this bone deviates, it doesn’t just create a bump; it destabilizes how you push off the ground. This instability can lead to secondary issues like peroneal tendonitis (inflammation of the tendons running along the outside of the ankle) or stress fractures if the weight distribution isn’t corrected.
Symptoms and Progression: ``Why is My Bunion Getting Bigger?``
It is very common for patients to visit a clinic complaining that “my bunion is getting bigger” and becoming increasingly red or swollen. This growth is often due to the formation of a bursa (a fluid-filled sac) or thick calluses as the skin tries to protect itself from shoe friction.
When diagnosing foot discomfort causes, podiatrists in the U.S. use the Coughlin Classification. This system helps determine if the issue is just an enlarged bone head or a more complex curvature of the entire fifth metatarsal. To get a clear picture, your doctor will take X-rays while you are standing to see how the bones shift under your actual body weight.
Advanced Diagnostic Markers
Conservative Relief: Orthotics, Support, and Better Shoes
Orthopedic Support and Inserts
Custom bunion foot inserts are one of the most effective tools available. These aren’t generic store-bought cushions; they are medical-grade devices designed to correct your specific gait. By stabilizing the foot, they take the pressure off the fifth metatarsal. For nighttime or extra stabilization, bunion support in the form of splints or toe spacers can help keep the toe in a more natural alignment.
Footwear and Topical Care
The ``Pillow`` Effect: Radiesse and Biologics
Surgical Excellence: The Best Way to Remove Bunions
Tailor’s Bunionectomy
A modern tailor’s bunionectomy involves a precise “osteotomy”—a controlled cut of the bone to shift it back into its correct anatomical position. Unlike traditional open surgeries that require large incisions, MIS is performed through tiny punctures (about 2-3mm).
Benefits of the MIS approach:
-
Minimal trauma: Lower risk of infection and less disruption to the blood supply.
-
No visible scarring: Most patients heal with barely a trace of the procedure.
-
Immediate Weight-Bearing: In many cases, you can walk in a “wedge” shoe the same day.
High-Tech Precision: 3D Planning and Robots
Top-tier clinics now use Patient-Specific Instrumentation (PSI). By taking a CT scan of your foot, surgeons can 3D-print a custom guide that fits onto your bone like a puzzle piece. This ensures the cut is made at the exact angle needed to narrow your foot perfectly. Some facilities also utilize robotic-arm assistance, which prevents the surgical burr from deviating even a fraction of a millimeter, ensuring the highest level of safety.
Recovery and Your Path to Success
After a tailor’s bunionectomy, American clinics follow a strict recovery protocol to ensure the bone heals perfectly.
The Four-Phase Recovery Protocol
-
The Protection Phase (Weeks 1-2): Keeping the foot elevated to reduce swelling. You will wear a surgical shoe to keep weight off the front of the foot.
-
The Mobilization Phase (Weeks 3-6): Transitioning into a walking boot. You may start gentle range-of-motion exercises to prevent stiffness in the pinky toe.
-
The Transition Phase (Weeks 6-12): Moving back into wide athletic sneakers. Physical therapy often begins here to strengthen the small muscles of the foot.
-
The High-Activity Phase (3-6 Months): Full return to running, jumping, and high heels (if desired).
The Impact of Nutrition and Lifestyle
During recovery, preventing a bunion recurrence is key. This includes maintaining a healthy weight to reduce load on the feet and ensuring adequate Vitamin D and Calcium intake for bone healing. Quitting smoking is also vital, as nicotine constricts blood vessels and can lead to a “non-union,” where the bone fails to knit back together.
By addressing the problem early with the help of a specialist, you can stop the pain, avoid secondary issues like arthritis, and get back to an active lifestyle with confidence.
Frequently Asked Questions
Is a tailor's bunion the same as a regular bunion?
Can I permanently get rid of a tailor's bunion without surgery?
How long is the recovery period for minimally invasive surgery (MIS)?
One of the greatest advantages of MIS is the rapid recovery. Most patients can walk immediately after the procedure in a specialized post-operative shoe or “wedge” boot. You will typically wear this protective footwear for about 2 to 4 weeks. Most patients return to regular sneakers by the 6th week and high-impact activities by the 3rd month.
Does insurance usually cover the cost of bunionette treatment?
In the United States, most major insurance providers cover both custom orthotics and surgical correction if the patient experiences documented pain and difficulty walking. Because a tailor’s bunion is a structural deformity that affects mobility, treatment is considered medically necessary rather than purely cosmetic.
What happens if I leave a tailor's bunion untreated?
If ignored, the constant pressure on the joint can lead to chronic bursitis, skin breakdown (ulceration), and eventually, osteoarthritis in the fifth metatarsal joint. Over time, the misalignment can also cause “transfer pain,” where other parts of your foot begin to hurt because they are overcompensating for the unstable lateral column.
Can I wear high heels again after the surgery?
Yes, the goal of the surgery is to return you to a full, active lifestyle. Once the bone has completely healed (usually confirmed by X-ray at the 3-to-6-month mark), you can return to fashion footwear. However, your podiatrist will likely suggest using a slim-profile orthotic and avoiding extremely narrow-pointed shoes to ensure the longevity of the surgical result.
References
-
Cleveland Clinic — Taylor’s Bunion (Bunionette): Causes, Symptoms & Treatment https://my.clevelandclinic.org/health/diseases/tailors-bunion-bunionette
-
Mayo Clinic — Bunions: Symptoms & Causes https://www.mayoclinic.org/diseases-conditions/bunions/symptoms-causes/syc-20354799
-
American Academy of Orthopaedic Surgeons (AAOS) — Bunionette (Tailor’s Bunion) https://orthoinfo.aaos.org/en/diseases–conditions/bunions/
-
Harvard Health — Bunions and Bunionettes Overview https://www.health.harvard.edu/bunions-and-bunionettes-overview
-
Hospital for Special Surgery (HSS) — Bunions: Hallux Valgus / Forefoot Pain https://www.hss.edu/health-library/conditions-and-treatments/list/bunions