This content is for informational purposes only and does not constitute medical advice. Please consult with a licensed podiatrist for a personalized evaluation and treatment plan. Individual results may vary.
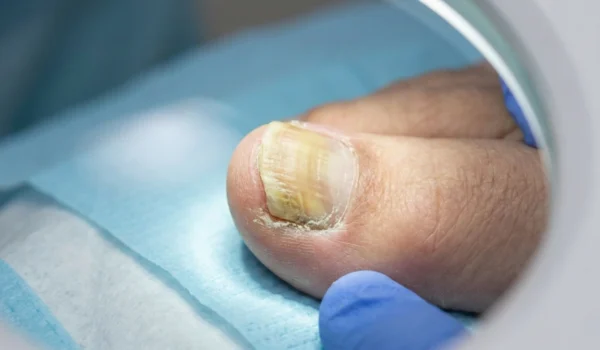
While there are several yellow toe nails causes, the most frequent reason is a fungal infection known as onychomycosis. This condition occurs when microscopic organisms, such as dermatophytes, enter the nail plate and begin to break down the keratin. A visit to a podiatrist is necessary if the nail becomes thick, painful, or changes color rapidly, as untreated infections can lead to permanent nail damage or spread to the skin and other toes.
Dr. Arkady Kaplansky specializes in the expert diagnosis and treatment of fungal foot infections in Los Angeles, utilizing the latest American podiatric protocols. His professional approach allows for the precise identification of the specific fungal strain, ensuring a customized recovery plan that restores the healthy appearance of the feet.
Epidemiology and Market Trends in the U.S. (2025–2026)
Recent data from 2025 and 2026 highlights a significant increase in fungal infections across the United States. According to the Centers for Disease Control and Prevention (CDC), fungal diseases now cause approximately 9 million outpatient visits annually. The economic impact is substantial, with direct medical costs for treatment reaching approximately $13.4 billion per year.
In Los Angeles and across Southern California, the prevalence of toenail fungus sits at about 14% of the general population. However, this number jumps to over 50% for adults aged 70 and older. The warm, humid climate of the region, combined with an active outdoor lifestyle, keeps the risk of infection high, making early intervention essential for residents.
What Causes the Infection? (Etiology and Transmission)
The primary yellow toenails cause is an invasion by dermatophytes, specifically Trichophyton rubrum. These organisms are highly adapted to surviving on human skin and nails by breaking down keratin.
Understanding how it spreads:
-
Nail fungus transmission: The infection spreads through direct skin-to-skin contact or by touching contaminated surfaces. Because toe nail fungus is contagious, it easily spreads between family members via shared towels, bath mats, or shower floors.
-
Environmental risks: In Los Angeles, the most common toenail fungus often thrives in damp environments like gym locker rooms, public pools, and the sandy areas of Santa Monica and Venice Beach.
Symptoms: How to Identify the Signs
Most patients seek professional help when they realize, “my toenails are thick and yellow.” The infection typically starts small—often as an isolated fungus pinky toenail—but gradually migrates to other toes.
Visible Signs to Watch For:
-
Discoloration: You may notice brown and yellow toenails or specific yellow toenails with lines (streaks running toward the cuticle).
-
Hyperkeratosis: The infection leads to thick yellow toenails or thick cloudy toenails that are difficult to trim.
-
Brittleness: Nails often become yellow and brittle toenails that crumble at the edges. In advanced stages, this can lead to severe decay, often referred to as nail rot.
-
Debris and Cavities: It is common to find soft white stuff under toenails, which is a buildup of fungal byproduct. In some cases, the infection eats away at the tissue, creating a hole in nail fungus or a hollow cavity under the plate.
Physical Sensations:
Modern Diagnostic Protocols
Because nearly 50% of nail deformities are caused by non-fungal issues like psoriasis or physical trauma, Dr. Kaplansky utilizes a multi-step diagnostic approach:
-
Microscopic Exam (KOH): Visualizing fungal structures under a microscope for immediate confirmation.
-
PCR Testing (Molecular Diagnosis): This advanced method identifies the exact DNA of the fungus within 24–48 hours, allowing for targeted therapy.
-
Clinical Evaluation: Distinguishing between fungal infection and “oil drop” spots characteristic of nail psoriasis.
Advanced Treatment Options in 2026
In 2026, the standard of care in Los Angeles has shifted toward combination therapy—removing infected debris while simultaneously killing the fungal spores.
Specialized Medications
Depending on the severity, Dr. Kaplansky may prescribe a powerful antifungal for nail infection. If a secondary bacterial infection develops due to deep cracks in the skin, an antibiotic for toe nail infection may be required to prevent complications like cellulitis.
High-Tech Laser Solutions
Los Angeles clinics favor laser technology because it avoids the liver-related side effects associated with oral pills:
-
Remy Laser and Cool Touch Varia: These lasers use focused light energy to heat the fungal colonies. The heat destroys the fungus (thermal lysis) without damaging the surrounding healthy skin.
-
Benefits: Laser treatment is painless, requires no downtime, and is highly effective at reaching spores deep within the nail bed.
The Onyfix Nail Correction System
If the fungal infection has caused the nail to curl or become ingrown, the Onyfix system is used. This is a painless, non-surgical correction method using a composite strip that retrains the nail to grow straight, avoiding the need for invasive procedures.
Surgical Intervention (Foot and Ankle Surgery)
In cases of total nail destruction or severe pain, a partial or full nail removal may be necessary. This allows the doctor to thoroughly clean the nail bed of all infected material, providing a “fresh start” for a new, healthy nail to grow.
Wound Care for High-Risk Patients
For Los Angeles residents living with diabetes, toenail fungus can lead to dangerous ulcers. Professional Wound Care at the clinic involves treating any skin breakdowns or bacterial infections to prevent systemic health risks.
CDC-Standard Prevention Tips
With recurrence rates as high as 50%, prevention is the final step of successful therapy:
-
Moisture Control: Wear moisture-wicking socks (synthetic or wool blends).
-
Shoe Rotation: Give your shoes 24–48 hours to dry out between uses and consider using UV shoe sterilizers.
-
Protection: Never walk barefoot in public showers, gyms, or around pool decks.
-
Tool Hygiene: Disinfect your nail clippers with alcohol after every use.
Treating toenail fungus early with an experienced podiatrist prevents the infection from spreading to others and restores the health and appearance of your feet.
Frequently Asked Questions
Why are my toenails turning thick and yellow?
This change is a common sign of a fungal infection where tiny organisms live and grow under the nail plate. Without professional treatment from a specialist like Dr. Arkady Kaplansky, the infection will likely get worse, causing the nail to crumble or even fall off.
Is toenail fungus contagious to my family?
Yes, it is very contagious and spreads easily through shared showers, towels, or bathroom mats. It is important to start treatment early to prevent passing the infection to other people in your household.
What is the fastest and safest way to get rid of the fungus?
Modern laser therapy, such as the Remy Laser, is a top choice because it kills the fungus with heat without the need for painful pills or downtime. If your nail is also curling or ingrown due to the infection, the Onyfix system can help it grow back straight without surgery.
Can I just wait for the fungus to go away on its own?
Unfortunately, toenail fungus will not disappear without medical help and usually becomes more difficult to treat over time. Early intervention is much easier and prevents the infection from spreading to all your other toes or causing permanent nail damage.
I have diabetes; is toenail fungus dangerous for me?
For people with diabetes, a thick fungal nail can press against the skin and cause hidden sores that lead to serious infections. Specialized podiatric exams and professional wound care are essential for diabetic patients to prevent these high-risk complications.
References
- Fungal Disease Burden by the Numbers | Fungal Diseases | CDC — https://www.cdc.gov/fungal/data-research/facts-stats/by-the-numbers.html
- Nail fungus – Symptoms and causes – Mayo Clinic — https://www.mayoclinic.org/diseases-conditions/nail-fungus/symptoms-causes/syc-20353294
- Nail fungus – Diagnosis and treatment – Mayo Clinic — https://www.mayoclinic.org/diseases-conditions/nail-fungus/diagnosis-treatment/drc-20353300
- Nail fungus: Diagnosis and treatment – American Academy of Dermatology — https://www.aad.org/public/diseases/a-z/nail-fungus-treatment
- Toenail Fungus – APMA — https://www.apma.org/patients-and-the-public/conditions-affecting-the-foot-and-ankle/toenail-fungus/
- Treatment Options for Onychomycosis: Efficacy, Side Effects, Adherence, Financial Considerations, and Ethics – PMC — https://pmc.ncbi.nlm.nih.gov/articles/PMC10941855/
- U.S. Dermatophytic Onychomycosis Treatment Market [2030] – Fortune Business Insights — https://www.fortunebusinessinsights.com/u-s-dermatophytic-onychomycosis-treatment-market-108477
- Onychomycosis Market Size to Hit USD 6.41 Billion by 2035 – Precedence Research — https://www.precedenceresearch.com/onychomycosis-market
- JUBLIA® (efinaconazole): For the treatment of toenail fungus — https://www.jubliarx.com/
- CPCPLAB068 – Onychomycosis Testing – Blue Cross Blue Shield (2026 Standards) — https://www.bcbsil.com/docs/provider/il/standards/cpcp/cpcplab/2026/cpcplab068-1-1-2026.pdf
- YAG laser in the treatment of toenail onychomycosis: a pilot study – PMC — https://pmc.ncbi.nlm.nih.gov/articles/PMC12552341/